|
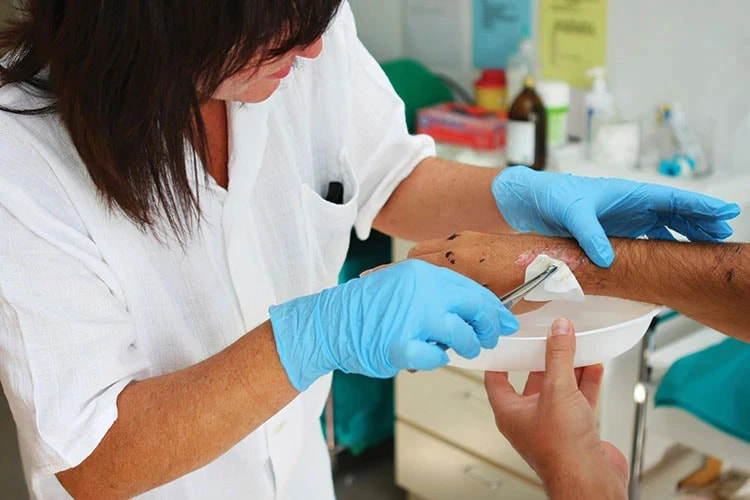
Wet-to-dry dressings have been used by wound care practitioners for decades as a standard wound treatment method for many wounds. However, in the present, this treatment method is being rarely used by surgeons and is getting outdated as it has various downsides. Take A Closer Look At Gauze DressingsWet-to-dry dressings are a non-selective type of mechanical debridement, a method of removing damaged or dead tissues from the wound. When wound care experts apply gauze dressing to cover a patient's wound, they are leaving a wet dressing on the wounds. When it gets dried, they take the dressing off gently and remove the dead tissues from the wound to accelerate the wound healing process. A gauze dressing is mostly used in treating wound drainage. There is a big debate in regards to the use of wet-to-dry dressings due to the use of gauze. It is a thin, translucent fabric that comes with a loose open weave structure to ensure stability. A wide variety of gauze dressings are available in the market to choose from. Some gauze dressings have a soft texture while some have rough where the little fibers of the gauze dressing can embed in the wounds and can make the condition worse. Downsides/Disadvantages of Using Gauze DressingThis form of mechanical debridement comes with several disadvantages. Some of them are as follows:
Despite the drawbacks of wet-to-dry dressings, it is still being used during the inflammatory stage of wound healing. It affects the healing process and also increases the risk of soft tissue infection and osteomyelitis. Alternatives to Wet-to-dry Wound Care DressingsThese days, wound care specialists are using impregnated forms of gauze dressings, such as gauze containing substances such as petroleum, honey, hydrogel, iodine, bismuth, and zinc. It can decrease the risks of trauma and prevent desiccation while changing the dressing. Clinicians are also using these dressings to prevent moisture loss from the wounds. They are readily available in the market. It can also be a cost-effective treatment method than using gauze as it cuts back the time required for the application of the dressings. While selecting an appropriate wound dressing, make sure that:
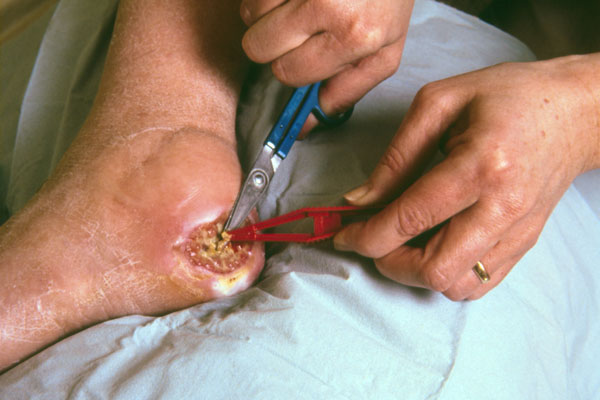
Debridement These are some other forms of debridement that can be used in the inflammatory stage of wound healing:
Dressings Gauze dressings require regular changes and are less effective in providing an optimal warm & moist environment to the wound. Earlier, when wet-to-dry dressings were used as a part of standard medical attention, they were considered as the most cost-effective wound care treatment plan, but today there are several options. Various suitable new dressings are available in the market.
These alternative dressings can boost the wound healing process, maintain a great level of moisture, protect wounds from possible infections and absorb high levels of drainage or stimulate tissue development as required. Modern dressings are non-adherent and speed up wound healing through maintaining a moist environment in the wound bed and are also convenient to the patients. Adapting advanced dressings and alternative debridement methods (apart from mechanical debridement ie. wet-to-dry dressings) as best wound care treatment can help wound care professionals quickly heal the wounds. Avoiding wet-to-dry dressings can result in cutting back healing time, decreasing infection risks, decreased healthcare visits as well as less pain while changing the dressing.
0 Comments
According to a study, chronic wounds affect over 7 million patients annually. When you have a wound which is painful & won’t heal in weeks or months, it can have a lasting impact on your daily routine. In this blog, we will explore why & when you should see the wound specialist near me and how an improved wound care treatment can help you reduce the risk of complications and ensure a faster, proper recovery. Keep reading to know: Wounds: The Basics Any wound is an injury to the living tissues where the skin is cut or broken. A simple crack or scrape in the skin leaves the underlying tissues exposed to foreign materials. Wounds can be the result of trauma, surgery, burns or infection. Minor wounds such as cuts, scrapes or punctures can be easily treated with traditional medical approaches to avoid infections. These traditional methods include appropriate dressings & therapies, debridements, minimally invasive & microsurgery and more. But when we say “Wound care”, it refers to a specialized type of treatment under the supervision of a Top wound care doctor near me who goes beyond the traditional approaches of a band-aid for minor cuts, scrapes or abrasions. They bring improved & advanced care to patients for wounds which are difficult to manage. Not all wounds are the same or heal within a significant amount of time. These wounds take months to heal and are known as chronic or non-healing. They typically result from underlying conditions such as poor blood flow, low oxygen, or circulation complexities in the legs from diabetes or prolonged pressure due to immobility etc. Chronic Wounds Include:
What Do Wound Care Specialists Do? A wound care specialist is a healthcare professional who undergoes a rigorous wound care training program to deal with chronic or non-healing wounds. While many primary care physicians are capable of treating minor wounds from a day-to-day injury, when it comes to chronic wounds, it takes the best wound care doctor near me to come up with a personalized treatment approach for a speedy recovery. Advancements offered by a wound care specialist include:
Benefits Of Seeing A Wound Doctor Near Me 1. Improved Care Coordination Though visiting hospital outpatient settings can have several benefits, it has some drawbacks, including a personalized patient experience. For example, a person suffering from a diabetic foot ulcer is referred to multiple professionals outside of the hospital, from radiology to vascular labs etc. It increases not only the period for the patients but also the costly & tiring procedure. On the other hand, with wound care near me, the patients can access a team of wound care experts under one facility having noticeable experience in their field. A multidisciplinary team of trained nurses, physicians and physical therapists has diverse clinical knowledge. They create a patient-focused treatment plan for effective healing. 2. Find The Root Cause With a Personalized Approach With a wound clinic near me, the patients get an individualized care plan using their knowledge & the conditions of the patient's wounds, health issues, underlying conditions, medical history and other references. Since the treatment is patient-focused, it is more likely to heal the wound more quicker. Additionally, the patients can have more resources to find the root cause of the symptoms that may slow the wound healing process, such as infection, diabetes, obesity, age, alcohol etc. 3. Advanced Technologies Wound care near me has access to the latest & advanced wound care technologies & treatments that patients may not find in a primary healthcare facility. They have the best equipment to offer various treatments, from specialised dressings to hyperbaric oxygen therapy. It can have a huge impact on a patient’s recovery. 4. Less Costly Compared to hospital visits, treating wounds from a <a href="https://www.woundcaresurgeons.org/">wound specialist near me</a> is less costly and more convenient in terms of multiple visits & medical expenses. Wrapping up Knowing the best possible treatment for chronic wounds can help avoid unnecessary medical complexities such as infection, amputation, etc. The top wound care doctor near me offers the most advanced solutions to treat open, infected & non-healing wounds. Book a bedside appointment now.
Visit us: https://www.woundcaresurgeons.org/ Pressure ulcers or pressure sores or bed sores are injuries to the skin and underlying tissue that occurs due to prolonged pressure on a particular part of the body, especially on the bony parts such as Heels, Elbows, and base of the spine, etc. It most commonly occurs in patients who spend most of their time in one place. For example, bedridden or confined to a wheelchair or people with other mobility issues, etc. It can develop over hours or days. If they are left untreated, it can lead to severe medical complications such as Infection, Amputation, etc. Are You Suffering From Any Of These Symptoms?Here are the warning signs of pressure wounds:
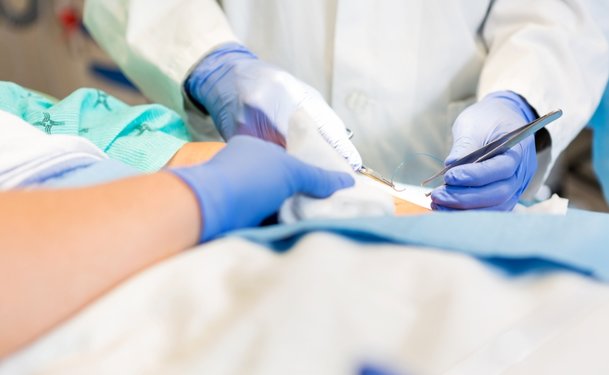
If a patient notices any of these symptoms, he/she should schedule a bedside appointment with a wound doctor. Post-operative surgical wound care not only helps keep the wounds infection-free but also promotes wound healing. So, when you are back home after going through surgery, keep an eye on the cuts or incisions made by the surgeons to look for the signs of infection, swelling, or bleeding. It will decrease the chances of any medical complications in the future. Therefore, it is important to follow the instructions provided by surgical wound consult to reduce scarring and limit the risk of infection. Take a look at some surgical wound care tips at home:What Is A Surgical Wound?Also known as an incision, it is a cut made in your skin during surgery. It can be sewed, stapled, taped, or glued together. They can vary in size and location but with proper care, they can sooner back to the normal stage. How To Take Care Of Surgical Wounds At Home?Surgical wounds take time to heal as they heal from the bottom to the top. If a patient has undergone surgery and is taking care of them at home, here are a few things to be considered. Take a look:
What Is A Chronic Wound?A wound is any type of injury or breakage in the skin or deep tissue. However, most of these wounds are minor or acute that heal on their own within a significant period like a few days or in some cases weeks if the injury is severe. But when acute wounds don’t heal properly within days or weeks or become infected, they are known as Chronic Wounds and require advanced medical care. In simple words, when acute wounds take longer than four weeks to heal after getting initial treatment, it becomes a chronic wound and requires wound care treatment California. In this blog, we will discuss everything that you need to know about chronic wounds. Let’s start first by knowing what causes a chronic wound: When Are The Chances Of Developing Chronic Wounds?A chronic wound can be a result of various reasons such as loss of blood circulation, infection, bacterial invasion, or inappropriate treatment. Or it can be due to extreme trauma. Other results include:
What Should I Do To Heal My Chronic Wounds Faster?To make a wound heal faster and properly, it is essential to follow some ground rules which are necessary for effective wound recovery. Keep in mind that the healing procedure is the same for all the wounds starting from building up new red tissue, closure of wound edges by new skin formation, and finally coverage of red tissue.
Here are the home care tips for chronic wounds that a patient needs to follow to help wounds heal faster and proper:
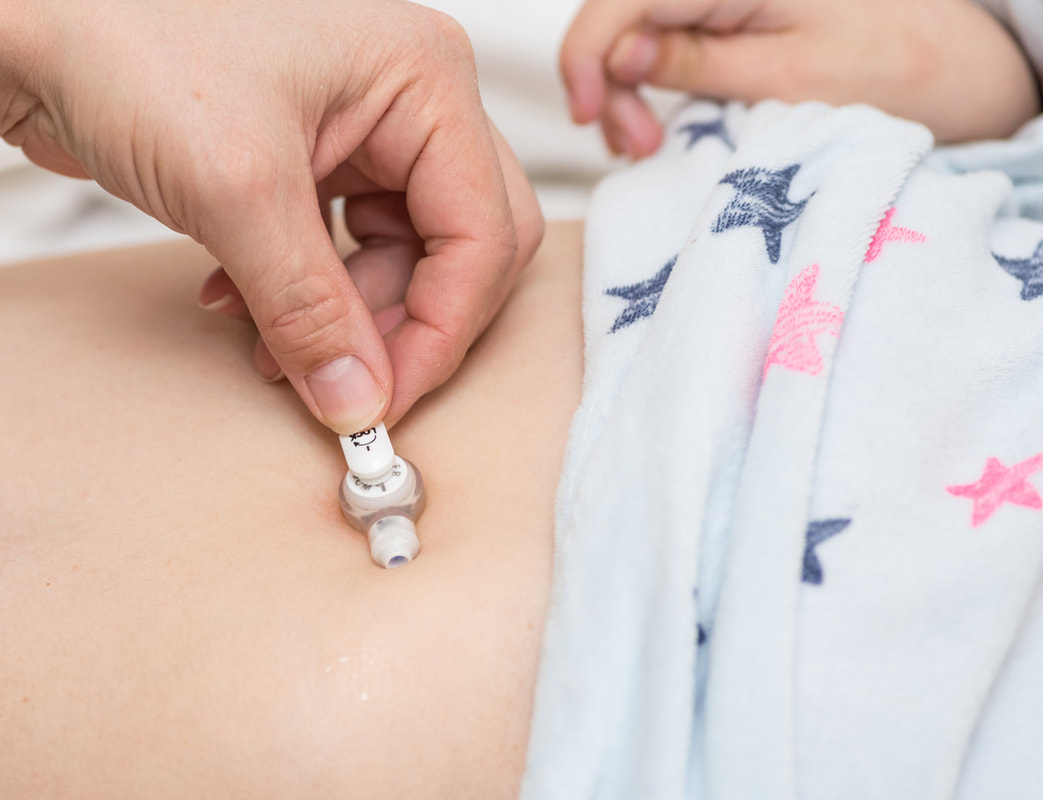
To avoid any upcoming complications or infections, it is vital to take very good care of chronic wounds such as diabetic or venous ulcers under the supervision of a venous leg ulcer specialist. They provide patients with a personalized treatment plan in their homes hence reducing the number of multiple visits to the hospitals. What Is A Gastrostomy Tube?A gastrostomy tube or let’s say a G-tube is a feeding tube that is placed through the abdomen and into the stomach to provide an alternative way of intaking food and/or medicines to the patients who have trouble eating. If a patient is unable to get enough food by mouth or in need of extra calories to grow, it requires surgery to insert a tube that further provides direct access to the patient’s stomach for feeding, hydration, or medication. A doctor or healthcare physician can recommend availing G Tube replacement service for a variety of medical conditions, but the most common is to enable patients to eat through a tube replacement. Who Needs A Gastrostomy Tube?Any patient who struggles to eat food and/or any type of supplemental medication directly from their mouth, due to the below reasons need a GTube replacement:
Risk factors that increase the eating disorders in patients include:
If you have just gone through surgery or have been suffering from any kind of acute or chronic wounds, your wound care surgeon might recommend you a wound vac therapy to heal the wound efficiently. But what is it? And how does it help treat patients? Read on to know. What is wound vac therapy?Also known as Negative Pressure Wound Therapy (NPWT), or vacuum-assisted closure therapy, a wound vac treatment is a method of treating the wounds using a special dressing connected to a battery-powered vacuum (suction) pump that sucks all the fluids and infections from the wound accelerate its healing speed. What happens during the wound vac procedure?During the wound vac treatment, the healthcare professionals apply a special bandage on the wound site which has an attached pump. It creates negative pressure on the open wound and pulls the edges of the wound together. Here, negative pressure means the patient experiences lower pressure over the wound than the pressure in the atmosphere. Before performing the therapy, the wound should be properly cleaned and dried. Advantages of using a wound vacIf any patient has a chronic or non-healing wound that takes a longer time to heal with traditional medical treatment, he/she must contact Wound care treatment California. The professional team of nurses, doctors & physicians visit the patient’s location & determine the type of treatment needed to heal a particular wound. The main concern of recommending a wound vac therapy is to increase the blood flow to the affected area so that the wound can heal quickly. Besides this increase in blood flow, the treatment has many other benefits such as:
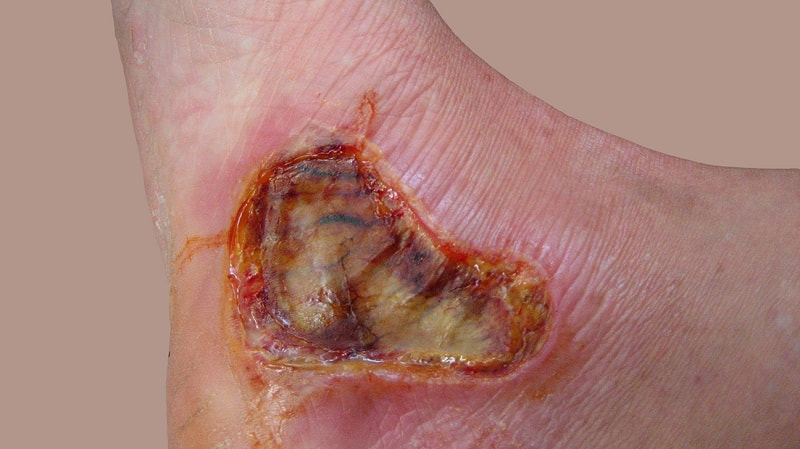
Patients with traumatic and surgical wounds, diabetic ulcers, burns, or bedsores should schedule a bedside appointment with a wound care specialist. The recommended length of a wound vac treatment takes changing the dressing every 48 to 72 hours or at least three times a week. A burn is an injury or damage to the skin caused by extreme heat, flame, or any contact with heated objects or chemicals. Depending on the severity, burns can vary from minor to life-threatening. Some burns only affect the upper layer of the skin but sometimes underlying tissues can also be severely affected. Clinically, they are characterized by degree, with first-degree being least severe and third-degree being most severe. Let’s know what third-degree burns are. What are Third Degree Burns?Third-degree burns or full-thickness burns are a type of burn that destroys the outer layer of the skin ie. epidermis and may damage the underlying tissues. They are extremely severe & painful than first or second-degree burns and may require skin grafting treatment. The burn site may have a white, grey, or brown appearance and the suffering patient requires immediate hospitalization for Burns And Scalds Wound Treatment. The treatment method may vary depending on the severity, extent, and location of the burn. Depending on the damage that occurred to the skin and surrounding tissues, doctors categorize burns into these categories:
What Causes Full-thickness (Third-degree) Burns?These types of burns are usually caused by any contact with one of the following:
What Are The Symptoms of Full-thickness (Third-degree) Burns?The following are the most common symptoms of third-degree burns:
How To Diagnose Full-Thickness (Third-Degree) Burns?The wound care professional team may conduct a series of physical tests to diagnose the depth, & severity of Full-thickness burns correctly. They may ask questions about the cause of the burn or whether the patient has any other medical conditions. The severity of the burns can be influenced by the patient's age, the percentage of total body surface area, and type of burn, etc. What Are The Treatment Options For Full-Thickness (Third-Degree) Burns?A person who suffers third-degree burns requires immediate hospitalization and treatment in a special burn unit. The treatment depends on the extent, severity, and location of the burn. Apart from that, the cause of the burn and the patient's overall health also determine a suitable treatment plan.
Here are the different treatment options used for Full-thickness (Third-degree) Burns:
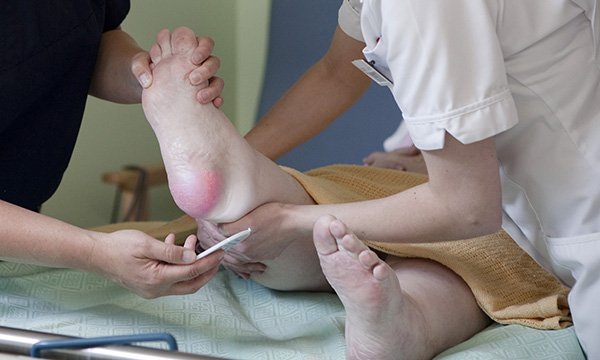
If a patient is bedridden or confined to a chair for a significant amount of time, he/she should be careful about the risks of developing Pressure Ulcers. It is a chronic, non-healing wound that can be difficult to treat and requires frequent positional changes, good hygiene, skincare as well as a healthy diet. What is a Pressure Ulcer?Also known as Bedsores, or Pressure Sores, pressure ulcers form where there is a long pressure on specific areas of the body and it results in the skin breaking down due to constant rubbing or pressing against a harder surface, such as a chair or bed. They can form anywhere but the most common body parts include elbows, knees, heels, tailbone, and ankles, etc. The lack of blood supply can cause the surrounding skin tissues to become damaged or die. Therefore, the people who:
If a patient is bedridden or notices any symptoms of Pressure Ulcer, they should immediately contact Pressure Ulcer Treatment Los Angeles. Preventing & Managing Pressure UlcerPressure ulcers can be managed and prevented efficiently by following a few steps we have shared here. Let’s have a look:
1. Promote Frequent Position Changes - Patients suffering from pressure ulcers are often advised by their surgeons/nurse practitioners to move or regularly change their position. It helps relieve the pressure on wounds that have already developed as well as helps prevent the formation of pressure ulcers. Doing a range of motion exercises also improves blood circulation. For example, a patient in a wheelchair should change their position every 15 minutes while in case of bed-confined, it can range about every 2 hours. Since pressure ulcers commonly occur on the tailbone, shoulders, or heels due to prolonged sitting, movement is essential. 2. Check Skin For Signs Of Pressure Ulcers - Pressure ulcers can be developed in a matter of a few hours. Therefore, the patients must check the skin daily for any signs of pressure ulcers. In case of any increased soreness and redness on any part of the body due to being in the same position, it becomes even more important. It could be a sign of Stage I Pressure Sore, but if the patient can move, & adjust position, the risks can be reduced. 3. Cleaning & Dressing - Pressure ulcer care & treatment depends on the severity of the wounds. Cleaning & dressing a wound includes the following:
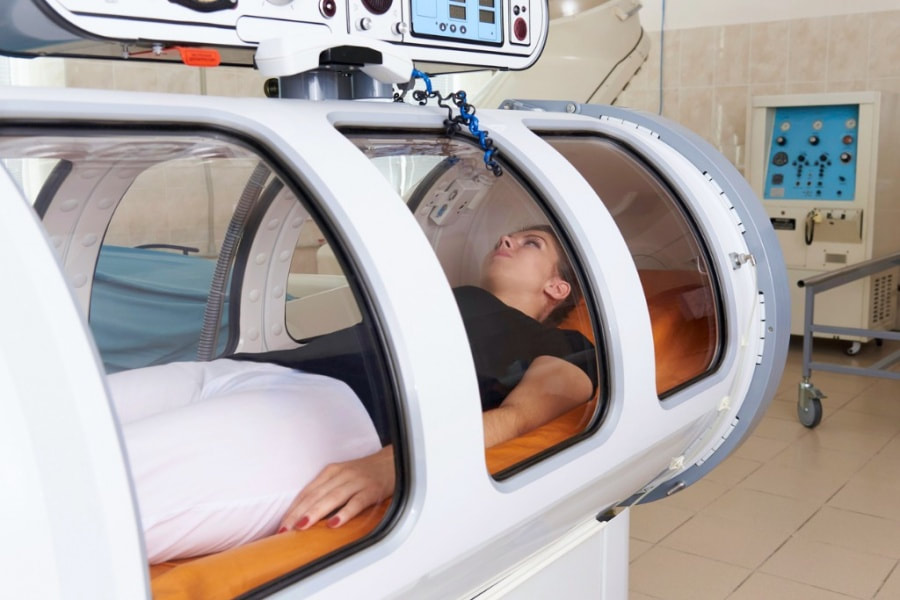
5. Use Specialty Bedding - The patients should use a mattress, bed, and cushions that help them sit or lie protectively. Depending on the need of the patient, the doctors may suggest specialty beds such as heel protectors, or special, cushioned padding to reduce the amount of pressure on affected areas of the body. 6. Keep the Skin Dry and Clean - Apart from these preventive measures, wound care Los Angeles also suggests patients to keep the skin clean and dry to avoid any infection. Incontinence is one of the biggest contributory factors in the development of pressure ulcers. When it gets combined with the limited ability to reposition, it increases the risk. Therefore, ointments and moisturizing creams are essential to create a barrier between the skin and infection. 7. Treat Chronic Health Conditions Effectively - Various chronic diseases can increase the risk of developing pressure ulcers. Some chronic diseases affect the functioning of the cardiovascular system and may result in poor blood circulation and increased risk of bedsores. Therefore, it is essential to treat chronic diseases on time and effectively to prevent the development or worsening of pressure sores. These are some tips that can be applied to reduce the risk of pressure ulcer development. Start implementing these tips as soon as possible if you have any signs of pressure ulcers and consult with wound care specialist Los Angeles for suitable medical treatment. Hyperbaric Oxygen Therapy or HBOT is a therapy that uses oxygen and air pressure to treat different kinds of injuries, from open wounds and severe burns to circulation issues & chronic wounds, etc. If any patient undergoes this therapy, they will be confined to a special chamber to breathe in pure oxygen in air pressure levels 1.5 to 3 times higher than the normal air pressure. This increased air pressure helps heal the wounds by filling the blood with enough oxygen, further repairing tissue, and restoring normal body functionalities. What Are The Benefits Of Hyperbaric Oxygen Therapy?HBOT therapy provides various benefits in treating severe wounds & injuries by delivering healing oxygen and thereby it is being increasingly adopted by Wound care professionals. Here are some of the benefits of HBOT therapy: 1. Treatment of Chronic Wounds - The very first & foremost use of HBOT therapy is that it helps with treating chronic, non-healing wounds which are taking too much time to heal due to many factors. For example, lack of oxygen, tissues aren’t being repaired faster, weaker immune system, and prolonged information tissue swelling. Here, HBOT therapy pushes oxygen into the tissues from outside. If there is no progress in wound healing, call your doctor and ask if HBOT therapy would help. 2. Improves Circulation - Effective blood circulation throughout the body is essential for overall health. It helps deliver oxygen to wounds and injuries while also removing toxins. One of the benefits of Hyperbaric Oxygen Therapy is that it increases circulation & oxygen flow throughout the body and helps accelerate the wound healing process. During the therapy, the lungs absorb much more oxygen than normal which is further absorbed into all of the body’s fluids and transports the oxygen and blood throughout the body. 3. Aids In Formation Of New Collagen - Hyperbaric oxygen therapy helps in the development of new collagen. It means it regenerates skin cells, connective tissue, and blood vessels. This is beneficial to the patients suffering from open wounds, injuries, burns, and skin grafts, etc. It floods the body with oxygen, helping faster wound healing rate, and allowing muscles and tissue to absorb oxygen. Due to this, they work more efficiently to regenerate themselves. 4. Boosts Immune System Response Against Infection - HBOT provides white blood cells with a large amount of oxygen to fight bacteria. This results in strengthening the immune system with the ability to fight off things that may cause an infection such as viruses etc. The therapy is helpful in cases when the patient is suffering from deep bone infections (osteomyelitis), brain abscesses, and chronic infections. It enhances the bone marrow’s ability to produce white blood cells as well as improves circulation throughout the body. Schedule a bedside appointment with Bedside Care Specialist USA and gather information.
5. Reduce Inflammation - Another benefit of HBOT therapy is that it helps with inflammation related to transplanted tissue, skin grafts, and reconstructive surgery as well as wounds caused by diabetes complications, etc. HBOT therapy is safe, but there are some side effects also. Thereby, the patients need to discuss with Bedside Specialist Care California. |

 RSS Feed
RSS Feed
